To scale the cliffs of the Amalfi Coast, to barter with street vendors at Christmas markets, to see The Pope say mass… There are a ton of reasons I book the trips I take (most involving food or scenery), but the latest was more personal. After over a year of watching prices, flights to Amsterdam dropped and my dream was within reach: in six short days, I was going to Dementia Village. “Hogeweyk” as it’s actually called (pronounced hoke-ah-waek) is a Truman Show-style village 20 minutes southeast of Amsterdam. Though seemingly ordinary, it is a constructed reality designed to cater to those with dementia. Everything about the community, from its layout and its shops to its antique décor and styles, is geared toward creating an environment that is as close to home as possible for all inhabitants. It is the currently the only one of its kind in the entire world, though others are excitedly following suit.
The purpose of this post is to paint as clear a picture as I can of the innovative, remarkable community that’s had my heart since its CNN debut. I will therefore try to keep it as simple and orderly as possible, refraining from writing too much about my feelings. 😉 As a lot of the information I’ve researched has been in other languages, some names or translations may sound funny. Bear with me as I try!
As I mentioned, Hogeweyk appears to be a disarmingly “normal” town. It’s tinier than we’re used to in the States and reminds me of a garden apartment complex or college campus. Its layout is intriguing; while secure, there are no walls or gates surrounding its perimeter. There are no locks, no guards, and no fence. Home to 152 residents, the tiny town boasts a restaurant, café, pub, supermarket, hair salon, music store, gym, lending agency for borrowing CDs and the like, various offices, and 23 “houses.” Each home is designed to match one of 7 different lifestyles:
- Urban/City Lifestyle: for those who were at the center of city life
- Homely Lifestyle: for those who value caring for their family and household
- Cultural Lifestyle: for those who love art and culture
- Indonesian Lifestyle: for those of Indonesian decent and whose daily life reflects their heritage
- Gooi/Well-to-Do Lifestyle: for those who find it essential to have proper manners, etiquette, and respected external appearances; for the “aristocratic Dutch” of a wealthier social class
- Traditional Lifestyle: for those whose pride and identity come from carrying out a traditional profession or managing a small business
- Christian Lifestyle: for those who live their lives according to their Christian faith
In general, each house is huge, with wide hallways, vast common areas, and personalized bedrooms. Floor-to-ceiling windows scan the length of each living room, and personal photos and art adorn the walls. Hardwood floors are found throughout, atop them beautiful furniture and antique accents. With resident reality orientation in mind, they match that which was popular in prior decades; Hogeweyk wants its environment to be virtually identical to that of residents’ past lives, focusing not only on religion and culture but also on smaller things like setup, music, style, and customs. It’s like an average US nursing home, except it’s the complete opposite. :-O
Homes cater to each lifestyle, however, and therefore differ in details and décor. The Indonesian apartments, for example, are decorated with flourishes of their indigenous culture. There are pictures of their homeland and color schemes to match. The food served is a mixture of Indonesian and Dutch cuisine, as residents identify with both cultures. Outside, gardens are planted “Eastern style” so that they’re suitable for prayer and meditation; they’re even equipped with big Buddha statues! Gooi houses, on the contrary, are super fancy; residents dine on lace tablecloths using fine glass and porcelain. Meals are brought to the table by “servants” who remain on standby out of sight. There are ornate chandeliers and formal relationships; servants (aka caregivers in disguise) are to be submissive and respectful.
Each resident’s lifestyle is determined prior to move-in based on preference and the results of a “digital lifestyle guide” via Motivaction, a research company that strives to pair people together according to their values, beliefs, and practices. You can actually go to their website and take the survey yourself; I did and it was spot-on! With an extensive wait-list, newcomers move first into an Admissions House where they’re catered to on a more individual level. Once a spot opens up in a lifestyle home of their choice, they’re able to settle in.
While residents seem to respond best when they retreat to private homes with likeminded neighbors, segregation is not maintained in outdoor life. Just as in a regular town, the streets and squares are neat and tree-lined. There are benches everywhere, as well as bikes for rent (no charge!) and pretty, calming fountains. There are no locks on any doors; all are free to roam about if and when they please, no matter the time of day. The town sits on nearly 4 acres, about half of which is actually built upon (homes are ~3,000ft2 each, with 5-7 bedrooms per home). There are tons of gardens, patios, and common areas, each with fresh flowers and one more beautiful than the next. Doors and windows are left propped open. What’s the catch, then? How is this community secured? Take a look at the somewhat confusing ground level floorplan (maybe this looks simple to you, but I’m a realtor, not an architect  ):
):
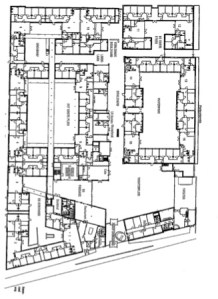
Though lots of open space and room to wander, apartments line the entire perimeter of the community. Aside from the single main entryway, there are no doors that lead outside of Hogeweyk. They all open up to areas within the village itself. As a result, locks are unnecessary.. wander guards are obsolete.. coded elevators are foolish. Not only are residents able to go out, they’re encouraged to. HALLELUJAH!
As was the case in Jim Carrey’s The Truman Show, however, residents are monitored 24/7 via video and audio surveillance. Around the clock care is provided by 240 “villagers” who are actually trained geriatric nurses and caregivers dressed in street clothes. Staff takes care of everything from cooking meals and planning activities to assisting with ADLs and administering meds. Even those working in various Hogeweyk businesses are trained in dementia care, down to the bartenders and theatre actors. No real money is exchanged, and if someone gets lost or becomes confused, there’s always a villager nearby to nonchalantly guide them home. If a nonna forgets she’s ordered coffee and begins to leave before it arrives, a neighbor affectionately joins her and encourages her to stick around. If a nonno steps out in the cold without his winter jacket, a friend will simply bring it out for him. Met with dignity and respect, neither scolded nor corrected, residents are happy, safe, and free. A favorite line I’ve read was spoken by Janette Spiering, one of the community’s directors, who said in reference to a resident who liked to garden: “The fact that he sometimes pulls out plants instead of weeds is not a problem. They can be replaced.” WOW.
Rather than summarize Hogeweyk’s list of daily activities, I wanted to share my unbiased experience of the community and what life appears to be like there. I arrived before 9AM; my flight landed at 7:30 and I immediately picked up my rental car and sped to Weesp (literally. I got a speeding ticket in the mail this afternoon 😐 ). Most residents were still at home, likely showering and getting ready for the day ahead. I spoke with Ellie at the entryway and gathered as much information from her as I could. She was a saint, and even drew me a map to help me find my way to Amsterdam when I left. ❤ She filled me in on some logistics and answered the questions I came prepared with:
- Similar to some communities here, there are three levels of care
- They’re referred to as assisting level, care level, and nursing level
- Technically, there is a ratio of ~1½ caregivers to 1 resident on any given day (~240:152)
- Overnight, there are 5 caregivers per level of care
- Instead of “making rounds,” they take turns watching the alarms and walking about the community, all remaining in contact with each other and allowing the residents to soundly sleep
- Homes are only worked in if there’s a clear reason for doing so (otherwise, they’re kept dark and quiet)
- If residents are up, caregivers may keep them company, as many prefer to just watch TV before heading to bed
- Most residents spend a substantial amount of time outside every single day
- Hogeweyk is open to anyone who wants to visit
- They want the neighborhood to be as normal as possible, and since the residents can’t leave, they want and encourage others to come in!
- There is a constant influx of visitors, none of whom are restricted to stuffy rooms or indoor common areas but can rather stroll through town, visit shops, participate in activities, and share a meal with their loved ones
- *Side Note* nursing home residents in the Netherlands go outside for an average of 96 seconds per day and 60% never receive visitors. Here in the US, 35% of dementia sufferers leave their homes just once a week, whether those homes are the ones they’ve lived in for years or an assisted living/memory care community. Even more heartbreaking, 10% go out only once a month. Obviously, this isn’t the case at Hogeweyk!
- The cost to build Hogeweyk was over $25 million, $22 million of which was funded by the Dutch government (and the rest by fundraising)
- It costs ~$7,000 per month to live in the community, though “care insurance” that Dutch citizens pay into for nearly all of their lives covers most, if not all, of that expense
- There is a perpetual waiting list to get in
- There are tons of different clubs and various activities, performances, festivals, and markets on a daily, weekly, or monthly basis
- Hogeweyk a pet friendly community (!!!!)
- Residents receive the care they need but the emphasis is on normal living, not their illness
- This method isn’t necessarily suitable for those with a heavy task-focused approach to caregiving, so they’re very selective about who they hire
- Management is required to do things differently, too; their vision must be recognized and implemented by all, with living, wellbeing, and care all interwoven in such a way that one cannot exist without the others
- It is important for all staff to communicate with residents both verbally and nonverbally
- Even if one is far into the disease process and cannot actively participate in or contribute to household activities, seeing, smelling, and listening to discussions about ordinary day-to-day things helps provide meaning
- They can still be involved and their plate of food doesn’t just appear out of nowhere!
- Everything is done on-site in each house and it’s communicated to the residents what’s going to be done, what they’re currently doing, and what tasks were just completed; they’re involved and informed verbally and with nonverbal cues
- Residents’ views of their caregiving “neighbors” differ according to their lifestyle
- Those from wealthier backgrounds think of them as servants, whereas people of working class origins believe they’re extended family members or friends
A million questions and thousands of hand gestures later (her English was così così), I had my long awaited tour. As I mentioned, nearly everyone was still in his or her apartment; I was able to galavant around town like a giddy tourist in awe of my surroundings. What struck me most was the normalcy of it all: there were shopping carts outside the supermarket, outdoor seats at the restaurant, and high-top tables at the pub. There were no unsightly med carts, no people dressed in scrubs, and no pull cords in the restrooms. It was memory care heaven. I won’t bore you with the details – the photos below speak for themselves. Just know that it was everything I’d dreamt of and then some.
After 3,655 miles of traveling, I figured it made no sense to tour and run. I wanted to immerse myself in Hogeweyk and take in as much as they’d allow me to. I sat outside of the café and introduced myself to some employees. Ok, fine.. I awkwardly inquired about where I could find coffee (dear God did I need it) and nonchalantly asked a hundred questions about their jobs. Welcoming is an understatement when describing Hogeweyk’s staff; from the house cleaners to the caregivers (& of course my girl Ellie at the entrance), they were beyond incredible. I chatted for a while with a younger man and thanked him profusely for his hospitality, insight, and espresso. I returned to my seat (in the sun, of course) and began taking notes.
Within a few moments, I was greeted by a cheerful resident who was “so happy to see me again.” I’m not worried about violating HIPAA laws (or whatever the Dutch equivalent may be) because I know I’m butchering these names, so I’ll call her what I heard her introduce herself as: Will. Will, like many residents, learned to speak English in school. We chatted as though we’d known each other for years, and I reciprocated my surprise and excitement to have bumped into her again. We talked about her family and how her father owns a hotel in Amsterdam. Will believes she’s in her 20s and still resides with her mom and dad. I asked ifs he’d like some coffee, and was happy to run inside and make her a cup. Upon my return, Will was gone; she’d likely been confused or forgotten I was coming back. The nice man I’d chatted with prior, however, had overheard our conversation and warmly accompanied Will to my table. He explained to her that I’d gone to get her coffee, and I melted at her response; she must’ve mentioned five times that she couldn’t believe her nice neighbor came to tell her that I (her friend) had gone to fix her a cup. Truthfully, I couldn’t believe it either. The Hogeweyk vision was obvious first in Ellie and reinforced continuously by everyone throughout the duration of my short (but valuable) stay.
Soon, there were three of us; another resident sat beside me, followed by a fourth, a fifth, and so on. Our table in the sun was packed and I was in my f’ing glory. Will was one of the few in our group who spoke English, but all were happy to converse despite our language barriers (and some obvious aphasia). Various members of the Hogeweyk staff walked by, but none passed without a friendly hello and brief exchange. Though evident enough in their overall demeanors, Will and her acquaintances assured me that they live in an incredible community with friendly, helpful neighbors. My heart was full and my head in the clouds.. how do we bring this place home?!
The remainder of my time was spent quietly observing life at Hogeweyk, and that’s exactly what I witnessed: living. In this tiny “fake” village, I saw true, unrestricted, happy, meaningful life. The innovation lies not only within the community’s design, but also (and primarily) in its approach. Hogeweyk is busting at its unlocked seams with compassion, dignity, freedom, and love. I can only hope to be part of such an incredible movement here in our own country one day.




































52.308051
5.040622






































